The Most Common 12 Heart Conditions – How to Spot Them Early and Reduce Risk
- BY Dr. Ajay Patel
- December 25, 2025
- 322 Views
This article is medically reviewed by Dr. Ajay Patel, MD, a Board-Certified Internal Medicine Physician (USA), for accuracy, clinical relevance, and adherence to current medical guidelines.
Heart conditions, heart disease symptoms, and early signs of heart problems are among the most searched health topics online because many cardiac issues begin silently. People often experience chest pain, shortness of breath, palpitations, or unusual fatigue long before a diagnosis is made. These symptoms are frequently ignored or misunderstood, which increases the risk of severe complications. Recognizing common heart conditions early allows timely testing, appropriate treatment, and meaningful risk reduction before permanent damage occurs.
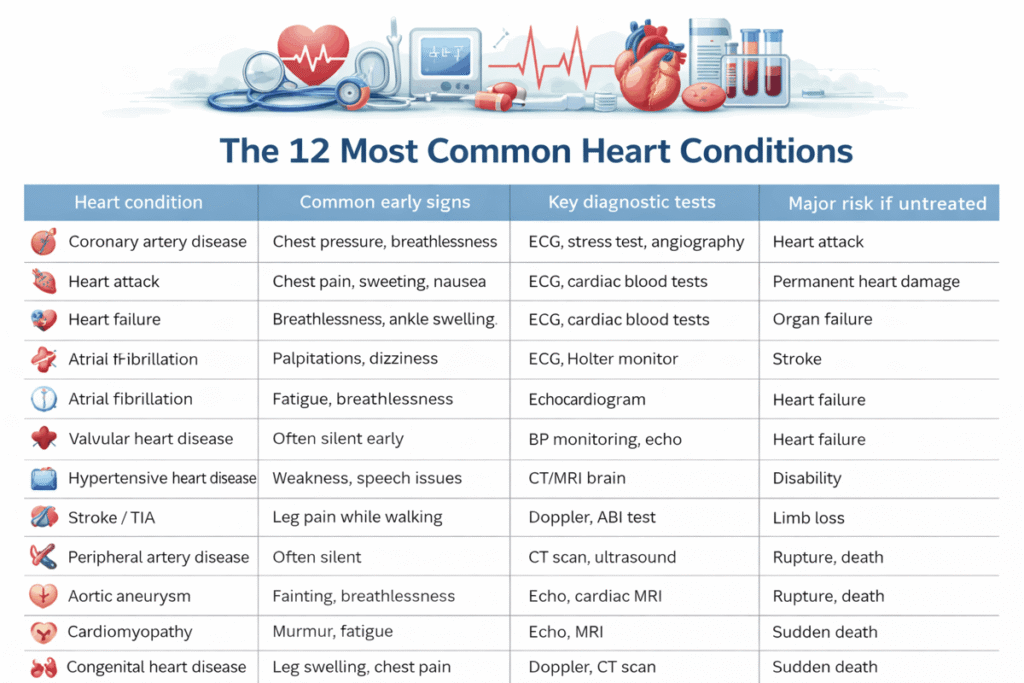
The following overview highlights the most frequently diagnosed and widely searched heart and cardiovascular conditions seen in routine medical practice.
| Heart condition | Common early signs | Key diagnostic tests | Major risk if untreated |
|---|---|---|---|
| Coronary artery disease | Chest pressure, breathlessness | ECG, stress test, angiography | Heart attack |
| Heart attack | Chest pain, sweating, nausea | ECG, cardiac blood tests | Permanent heart damage |
| Heart failure | Breathlessness, ankle swelling | Echocardiogram, blood tests | Organ failure |
| Atrial fibrillation | Palpitations, dizziness | ECG, Holter monitor | Stroke |
| Valvular heart disease | Fatigue, breathlessness | Echocardiogram | Heart failure |
| Hypertensive heart disease | Often silent early | BP monitoring, echo | Heart failure |
| Stroke / TIA | Weakness, speech issues | CT/MRI brain | Disability |
| Peripheral artery disease | Leg pain while walking | Doppler, ABI test | Limb loss |
| Aortic aneurysm | Often silent | CT scan, ultrasound | Rupture, death |
| Cardiomyopathy | Fainting, breathlessness | Echo, cardiac MRI | Sudden death |
| Congenital heart disease | Murmur, fatigue | Echo, MRI | Heart failure |
| DVT / Pulmonary embolism | Leg swelling, chest pain | Doppler, CT scan | Sudden death |
Coronary Artery Disease (CAD)
What it is
Coronary artery disease develops when the arteries supplying blood to the heart muscle become narrowed due to plaque buildup. These plaques form gradually from cholesterol and inflammatory material, reducing blood flow to the heart. This condition is the most common cause of heart attacks and one of the leading contributors to long-term heart disease.
Top early signs
Early symptoms often appear during physical activity and improve with rest. Common signs include chest pressure or tightness, shortness of breath while walking, reduced stamina, and unexplained fatigue. Many people describe discomfort rather than sharp pain, which leads to delayed medical evaluation.
Key tests
Diagnosis usually begins with an electrocardiogram to assess heart rhythm. Blood tests evaluate cholesterol and cardiovascular risk markers. Stress testing helps detect reduced blood flow during exertion. Imaging tests such as coronary angiography confirm the extent of artery narrowing.
First-line treatment
Treatment focuses on slowing plaque progression and preventing complications. Medications are used to control cholesterol, blood pressure, and clot formation. Lifestyle changes play a central role. In advanced cases, stents or bypass surgery may be required.
Red flags
Chest pain at rest, pain spreading to the arm or jaw, sudden breathlessness, or collapse require immediate emergency care.
Heart Attack (Myocardial Infarction)
What it is
A heart attack occurs when a coronary artery becomes suddenly blocked, stopping blood flow to part of the heart muscle. This blockage is usually caused by a blood clot forming over a ruptured plaque. Without rapid treatment, heart muscle damage becomes permanent.
Top early signs
Severe chest pain or pressure is the most recognized symptom. Other signs include sweating, nausea, vomiting, and shortness of breath. Many women experience atypical symptoms such as extreme fatigue, dizziness, upper back discomfort, or indigestion-like sensations. People with diabetes may experience minimal pain.
Key tests
Diagnosis relies on urgent electrocardiograms and cardiac blood tests that detect heart muscle injury. Imaging procedures identify the blocked artery and guide emergency care.
First-line treatment
Immediate hospital treatment is essential. Restoring blood flow quickly is the priority, followed by long-term medications and structured recovery programs.
Red flags
Chest pain lasting more than a few minutes, collapse, or severe breathlessness signals a medical emergency.
Heart Failure
What it is
Heart failure occurs when the heart cannot pump blood efficiently enough to meet the body’s needs. It often develops after long-standing coronary artery disease, high blood pressure, or previous heart attacks. Fluid buildup and reduced circulation are key features.
Top early signs
Early signs include breathlessness during routine activity, swelling of the ankles or legs, rapid weight gain from fluid retention, and persistent fatigue. Difficulty breathing when lying flat is common.
Key tests
Doctors use echocardiograms to assess pumping strength, blood tests to evaluate cardiac stress, and imaging to detect fluid accumulation.
First-line treatment
Management focuses on reducing fluid overload, supporting heart function, and controlling underlying causes. Medications and daily symptom monitoring are essential.
Red flags
Sudden worsening breathlessness, confusion, chest pain, or fainting require urgent medical attention.
Atrial Fibrillation and Other Arrhythmias
What it is
Atrial fibrillation is the most common type of heart rhythm disorder, also known as an arrhythmia. It occurs when the electrical signals in the upper chambers of the heart become chaotic, causing the heart to beat irregularly and often too fast. Other arrhythmias include supraventricular tachycardia, ventricular tachycardia, and bradycardia, each affecting how efficiently the heart pumps blood.
Because atrial fibrillation can be intermittent or silent, many people live with it for years without a diagnosis. Despite this, it significantly increases the risk of stroke and heart failure if left untreated.
Top early signs
Palpitations are the most frequently reported symptom and are often described as fluttering, pounding, or an irregular heartbeat. Some people notice shortness of breath, fatigue, lightheadedness, or reduced exercise tolerance. Others experience chest discomfort or anxiety-like sensations. A large number of individuals have no noticeable symptoms and only discover the condition during routine health checks, which is why searches for irregular heartbeat symptoms are so common.
Key tests
An electrocardiogram is the primary test used to confirm atrial fibrillation and other arrhythmias. Because irregular rhythms may come and go, doctors often recommend longer monitoring using Holter devices or event recorders. Echocardiograms help assess heart structure and rule out underlying valve or muscle problems. Blood tests may be ordered to check thyroid function and electrolyte levels.
First-line treatment
Treatment depends on symptom severity and stroke risk. Medications are commonly prescribed to control heart rate or restore normal rhythm. Blood-thinning medicines are often required to reduce the risk of stroke. In some cases, electrical cardioversion or catheter-based procedures are used to correct abnormal electrical pathways. Lifestyle changes, including limiting alcohol and managing stress, also play an important role.
Red flags
Sudden fainting, severe chest pain, signs of stroke such as weakness or speech difficulty, or a rapid heartbeat with dizziness require immediate medical evaluation.
Valvular Heart Disease
What it is
Valvular heart disease occurs when one or more heart valves do not open or close properly. This leads to disrupted blood flow within the heart and increased strain on the heart muscle. Common valve problems include aortic stenosis, mitral regurgitation, and mitral valve prolapse.
Valve disease may develop due to aging, infections, rheumatic fever, or congenital abnormalities. Many cases progress slowly, which explains why people often search for valve disease symptoms only after noticeable changes in stamina or breathing appear.
Top early signs
Early symptoms often include breathlessness during activity, fatigue, and reduced exercise capacity. Some people experience palpitations, chest discomfort, or swelling in the legs. Fainting episodes may occur in severe valve narrowing, particularly during exertion. In mild cases, symptoms may be absent for years, even while heart damage progresses.
Key tests
Echocardiography is the most important test for diagnosing valvular heart disease, as it provides detailed images of valve movement and blood flow. Doctors also use physical examination to detect heart murmurs. Electrocardiograms help assess rhythm changes, while chest imaging may show heart enlargement in advanced cases.
First-line treatment
Management depends on the severity of valve dysfunction. Mild cases may only require regular monitoring and symptom control. Medications can help manage fluid buildup, blood pressure, and rhythm issues. When valve damage becomes severe, repair or replacement through surgical or minimally invasive procedures may be required to prevent heart failure.
Red flags
Sudden fainting, rapidly worsening breathlessness, chest pain during activity, or new swelling of the legs signal advanced disease and require urgent cardiology assessment.
Hypertensive Heart Disease
What it is
Hypertensive heart disease refers to changes in the heart caused by long-standing high blood pressure. When blood pressure remains elevated over time, the heart must work harder to pump blood. This leads to thickening of the heart muscle, reduced relaxation, and eventual weakening of heart function.
This condition is particularly common because high blood pressure often produces no early symptoms. Many people search for high blood pressure heart damage only after complications develop.
Top early signs
In the early stages, hypertensive heart disease may cause no noticeable symptoms. As the condition progresses, individuals may experience breathlessness during activity, chest discomfort, fatigue, palpitations, or swelling in the lower limbs. Headaches and dizziness may also occur when blood pressure is poorly controlled.
Key tests
Diagnosis begins with repeated blood pressure measurements. Electrocardiograms help identify heart muscle thickening, while echocardiograms provide detailed information about heart structure and pumping function. Blood tests are often used to assess kidney health and other organs affected by high blood pressure.
First-line treatment
The cornerstone of treatment is consistent blood pressure control. Medications are prescribed to lower blood pressure and reduce strain on the heart. Lifestyle changes such as reducing salt intake, maintaining a healthy weight, regular physical activity, and limiting alcohol consumption are essential. Early treatment can slow or reverse heart changes in many cases.
Red flags
Severely elevated blood pressure accompanied by chest pain, breathlessness, confusion, or vision changes requires immediate medical attention.
Stroke and Transient Ischemic Attack (TIA)
What it is
A stroke occurs when blood flow to part of the brain is interrupted, either due to a blocked artery or bleeding within the brain. When brain cells are deprived of oxygen, they begin to die within minutes. A transient ischemic attack, often called a mini-stroke, is caused by a temporary blockage that resolves on its own but serves as a serious warning sign of a future stroke.
Stroke is closely linked to heart conditions because problems such as atrial fibrillation, coronary artery disease, and high blood pressure significantly increase stroke risk.
Top early signs
Early stroke symptoms usually appear suddenly. Common signs include weakness or numbness on one side of the body, difficulty speaking or understanding speech, facial drooping, sudden vision loss in one or both eyes, dizziness, and loss of balance. Many people search online for these symptoms because they appear without pain and are often confusing or frightening.
A transient ischemic attack produces similar symptoms, but they resolve within minutes or hours. Even when symptoms disappear, the risk of a full stroke remains high.
Key tests
Emergency brain imaging such as CT scans or MRI is used to determine whether a stroke is caused by blockage or bleeding. Additional tests may include carotid artery ultrasound to detect narrowed neck arteries, heart rhythm monitoring to identify irregular heartbeats, and blood tests to assess clotting and risk factors.
First-line treatment
Treatment depends on the type of stroke. Blockage-related strokes may require clot-dissolving medications or procedures to remove clots if treatment is received quickly. Long-term care focuses on preventing recurrence through blood-thinning medications, blood pressure control, cholesterol management, and treatment of underlying heart conditions.
Red flags
Sudden weakness, slurred speech, vision loss, or confusion are medical emergencies. Immediate hospital care is essential, as early treatment can prevent permanent disability or death.
Peripheral Arterial Disease (PAD)
What it is
Peripheral arterial disease occurs when arteries supplying blood to the legs and arms become narrowed due to plaque buildup. It is caused by the same process that leads to coronary artery disease, but it affects the limbs instead of the heart. PAD is a strong indicator of widespread cardiovascular disease and increased risk of heart attack and stroke.
Many people remain unaware they have peripheral arterial disease until symptoms interfere with daily activities.
Top early signs
The most common early symptom is leg pain or cramping during walking that improves with rest, a condition known as claudication. Other signs include cold feet, numbness, slow-healing wounds on the legs or feet, and changes in skin color. Some individuals experience weakness or heaviness in the legs rather than pain.
Because these symptoms are often mistaken for muscle strain or aging, diagnosis is frequently delayed.
Key tests
Doctors use physical examination and simple tests to assess blood flow. An ankle-brachial index compares blood pressure in the ankle and arm to detect reduced circulation. Doppler ultrasound helps visualize blood flow in the leg arteries. In advanced cases, CT or MR angiography may be used.
First-line treatment
Treatment focuses on improving circulation and reducing cardiovascular risk. Smoking cessation is critical. Medications may be prescribed to prevent clot formation and manage cholesterol. Supervised exercise programs are highly effective in improving walking distance. In severe cases, procedures to open blocked arteries may be necessary.
Red flags
Severe leg pain at rest, non-healing ulcers, skin discoloration, or sudden coldness of a limb require urgent medical attention, as they may signal critical limb ischemia.
Aortic Aneurysm and Aortic Dissection
What it is
An aortic aneurysm is an abnormal bulging or weakening of the aorta, the largest artery in the body. Over time, the weakened area can expand and eventually rupture. An aortic dissection occurs when a tear develops in the inner wall of the aorta, allowing blood to flow between layers of the vessel wall. Both conditions are life-threatening and often linked to high blood pressure, smoking, and inherited connective tissue disorders.
Many people are unaware they have an aortic aneurysm until it is discovered incidentally or causes complications.
Top early signs
Aortic aneurysms often produce no symptoms in the early stages. As they enlarge, individuals may experience deep, persistent chest, back, or abdominal discomfort. Aortic dissection causes sudden, severe pain described as tearing or ripping, often radiating to the back or legs. Dizziness, fainting, or sudden weakness may occur.
Searches for sudden chest and back pain often reflect concern about this condition due to its dramatic presentation.
Key tests
Imaging plays a central role in diagnosis. Ultrasound is commonly used to screen for abdominal aortic aneurysms. CT angiography and MRI provide detailed images of the aorta and are essential for diagnosing dissections and determining severity.
First-line treatment
Management depends on size and risk. Small aneurysms may be monitored regularly with imaging and strict blood pressure control. Larger aneurysms or dissections often require urgent surgical or endovascular repair. Long-term treatment includes blood pressure management and avoidance of activities that strain the aorta.
Red flags
Sudden severe chest or back pain, collapse, shortness of breath, or signs of shock are medical emergencies that require immediate hospital care.
Cardiomyopathy
What it is
Cardiomyopathy refers to diseases of the heart muscle that make it harder for the heart to pump blood effectively. The most common forms include dilated cardiomyopathy, hypertrophic cardiomyopathy, and restrictive cardiomyopathy. These conditions may be inherited, develop after viral infections, or arise due to long-term heart stress from high blood pressure or alcohol use.
Cardiomyopathy is a frequent cause of heart failure and sudden cardiac death, especially in younger individuals and athletes, which is why symptoms related to fainting and exercise intolerance are widely searched.
Top early signs
Early symptoms vary by type but often include breathlessness during activity, unusual fatigue, chest discomfort, palpitations, and dizziness. Some people experience fainting spells, particularly during exertion. In early stages, symptoms may be mild or absent, allowing the condition to progress unnoticed.
Key tests
Diagnosis typically involves echocardiography to evaluate heart muscle thickness, chamber size, and pumping strength. Cardiac MRI provides detailed structural information. Electrocardiograms help detect rhythm abnormalities, and genetic testing may be recommended when inherited forms are suspected.
First-line treatment
Treatment depends on the type and severity of cardiomyopathy. Medications are commonly used to support heart function, control rhythm disturbances, and reduce fluid buildup. Lifestyle adjustments such as limiting alcohol and avoiding intense physical strain are important. Some patients may require implantable devices to prevent life-threatening rhythm problems.
Red flags
Fainting during physical activity, worsening breathlessness, chest pain, or a family history of sudden cardiac death require urgent cardiology evaluation.
Congenital Heart Disease in Adults
What it is
Congenital heart disease includes structural heart abnormalities present from birth. Advances in medical care allow most affected individuals to survive into adulthood, but many continue to face long-term complications. Some congenital heart defects remain undetected until adulthood, when symptoms finally appear.
Adult congenital heart disease is increasingly common and often misunderstood, leading many people to search for symptoms later in life.
Top early signs
Symptoms depend on the specific defect but often include shortness of breath, fatigue, reduced exercise tolerance, heart murmurs, and irregular heartbeats. Some adults experience bluish discoloration of lips or fingertips during exertion. Others may have no symptoms until stress on the heart increases with age.
Key tests
Echocardiography is the primary diagnostic tool. Cardiac MRI and CT scans provide detailed anatomical information. Electrocardiograms help detect rhythm issues, and specialized testing may be required in adult congenital heart clinics.
First-line treatment
Management focuses on long-term monitoring and prevention of complications. Some individuals require medications to support heart function, while others may need corrective or repeat procedures. Regular follow-up with specialists is essential to manage evolving risks.
Red flags
Sudden worsening breathlessness, fainting, cyanosis, or new rhythm disturbances require immediate medical attention.
Deep Vein Thrombosis and Pulmonary Embolism
What it is
Deep vein thrombosis occurs when a blood clot forms in a deep vein, most commonly in the legs. If part of the clot travels to the lungs, it causes a pulmonary embolism, a life-threatening condition. Together, these are known as venous thromboembolism and are closely linked to cardiovascular health.
Risk increases with prolonged immobility, surgery, cancer, pregnancy, smoking, and certain heart conditions.
Top early signs
Deep vein thrombosis often presents with one-sided leg swelling, pain, warmth, and redness. Pulmonary embolism symptoms include sudden shortness of breath, chest pain that worsens with breathing, rapid heartbeat, dizziness, or collapse. Because symptoms can appear suddenly, many people search urgently for answers online.
Key tests
Diagnosis includes blood tests that assess clot activity, ultrasound imaging of the legs, and CT scans of the lungs when pulmonary embolism is suspected. Heart monitoring may be performed to assess strain on the heart.
First-line treatment
Treatment focuses on preventing clot growth and recurrence. Blood-thinning medications are the mainstay of therapy. In severe cases, clot-removal procedures or intensive care support may be required. Preventive strategies include mobility, hydration, and managing risk factors.
Red flags
Sudden breathlessness, chest pain, coughing blood, or collapse are medical emergencies and require immediate hospital care.
Common Questions People Ask About Heart Conditions
Chest discomfort, shortness of breath, palpitations, unexplained fatigue, and swelling of the legs are common early warning signs.
Heart-related pain often feels like pressure or heaviness, may spread to the arm or jaw, and can occur with sweating or breathlessness.
Yes. Conditions such as high blood pressure, atrial fibrillation, and cardiomyopathy may progress silently for years.
Persistent chest discomfort, repeated palpitations, unexplained breathlessness, fainting, or a strong family history of heart disease warrant evaluation.
Women often experience fatigue, dizziness, nausea, back or jaw discomfort rather than classic chest pain.
Evaluation commonly includes electrocardiograms, blood tests, echocardiography, and imaging based on symptoms.
Some early changes can be improved with treatment and lifestyle changes, but advanced damage usually requires long-term management.
Irregular heart rhythm, high blood pressure, smoking, diabetes, and untreated valve disease increase stroke risk.
Yes. It may indicate peripheral arterial disease, which is linked to higher heart attack and stroke risk.
It forces the heart to work harder, leading to thickened heart muscle and eventual heart failure.
Some are harmless, but others increase the risk of stroke or sudden cardiac arrest and require treatment.
Seek emergency medical care immediately, as early treatment can be life-saving.
Conclusion
Heart conditions often develop gradually, but their impact can be sudden and severe when early warning signs are missed. Chest discomfort, shortness of breath, palpitations, fatigue, leg swelling, or sudden neurological symptoms should never be ignored, as they may signal an underlying cardiovascular problem. The most common heart conditions share many risk factors and symptoms, which is why timely evaluation and proper testing are so important.
Early identification allows doctors to start appropriate treatment before permanent damage occurs. Managing blood pressure, cholesterol, blood sugar, body weight, and lifestyle habits plays a critical role in reducing long-term risk. Regular health checkups, awareness of family history, and prompt medical attention for unusual symptoms can significantly lower the chances of heart attacks, strokes, and heart failure.
Protecting heart health is not about reacting to emergencies alone; it is about recognizing changes early and taking consistent action. With informed decisions, medical guidance, and ongoing care, many heart conditions can be controlled effectively, allowing people to maintain an active and healthier life.








