Female Pattern Hair Loss: When to Consider a Transplant vs Medical Treatment
- BY Dr. Ajay Patel
- December 21, 2025
- 572 Views
This article is medically reviewed by Dr. Ajay Patel, MD, a Board-Certified Internal Medicine Physician (USA), for accuracy, clinical relevance, and adherence to current medical guidelines.
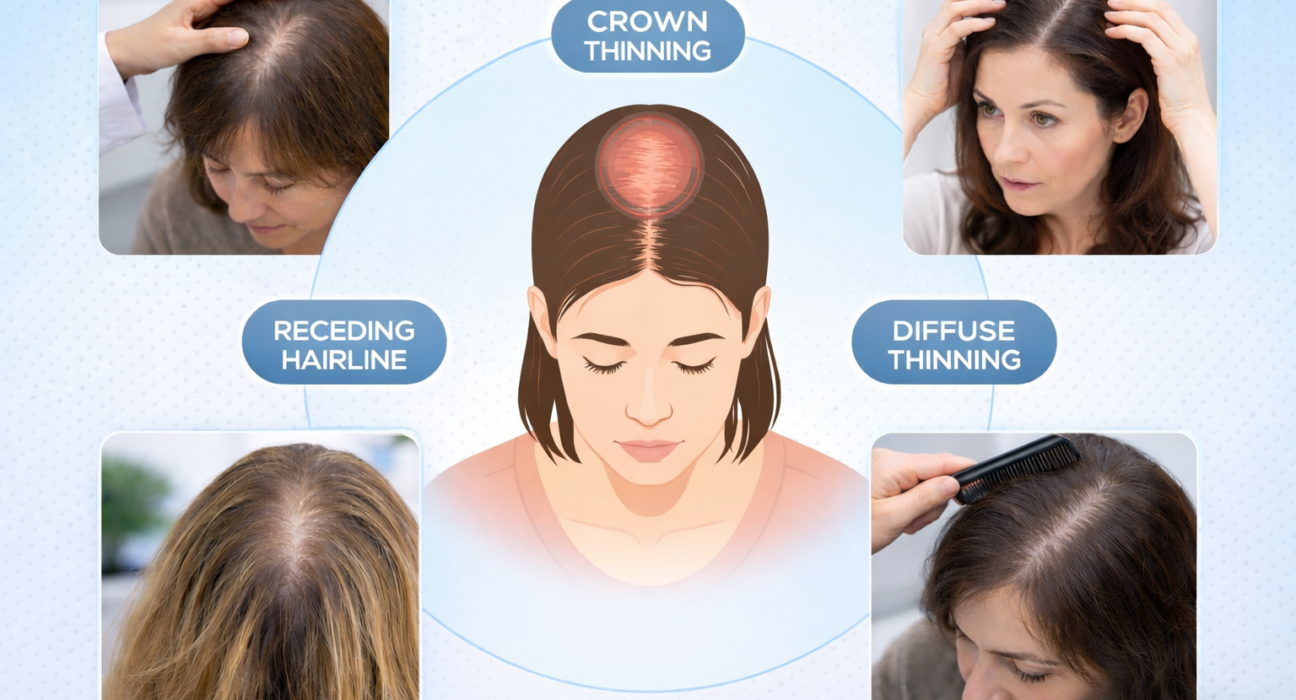
Female pattern hair loss is one of the most common causes of progressive hair thinning in women. Many women notice a widening part, reduced hair volume, or visible scalp over the crown. These changes often start slowly. They worsen over time if left untreated. Early understanding helps women choose the right treatment and avoid unnecessary procedures.
What Is Female Pattern Hair Loss?
Female pattern hair loss (FPHL) is a genetic and hormone-related condition. It causes gradual thinning over the crown and mid-scalp. Unlike male baldness, women rarely develop complete bald patches. The frontal hairline usually stays intact. Hair density reduces across a wider area.
This condition also goes by the name female androgenetic alopecia. It affects women of all ages. The risk increases after menopause. Family history plays a major role.
Medical studies and clinical guidelines from organizations like International Society of Hair Restoration Surgery and Cleveland Clinic confirm that FPHL is progressive. Early treatment improves long-term outcomes.
How Female Pattern Hair Loss Usually Starts
Most women do not notice sudden hair loss. The process remains slow and subtle. Common early signs include:
- Widening of the central hair part
- Reduced ponytail thickness
- Increased hair shedding during washing
- Scalp visibility under bright light
- Loss of volume around the crown
Hair follicles shrink over time. Each growth cycle produces thinner strands. Eventually, some follicles stop producing visible hair.
Why Female Pattern Hair Loss Happens
FPHL develops due to a combination of internal and external factors. Genetics remains the strongest cause. Hormonal sensitivity also plays a key role.
Main Causes Include:
- Genetic predisposition
- Sensitivity to androgens (DHT)
- Estrogen decline during menopause
- Aging of hair follicles
- Chronic inflammation of the scalp
Hormonal imbalance alone does not cause hair loss. The scalp’s sensitivity to hormones matters more than hormone levels.
Conditions That Can Worsen Hair Thinning
Doctors must rule out reversible causes before planning long-term treatment. Many women experience temporary hair loss that mimics FPHL.
| Condition | Effect on Hair |
|---|---|
| Iron deficiency | Weakens hair roots |
| Thyroid disorders | Disrupts growth cycles |
| Post-pregnancy shedding | Temporary diffuse loss |
| Crash dieting | Nutrient deficiency |
| Chronic stress | Triggers telogen effluvium |
Treating these conditions can improve hair density. Surgery is not recommended until doctors confirm true FPHL.
How Doctors Diagnose Female Pattern Hair Loss

Accurate diagnosis decides the treatment path. Doctors rely on clinical examination and history. They avoid rushing into procedures.
Diagnosis Includes:
- Scalp examination under magnification
- Pattern analysis using the Ludwig scale
- Hair pull test to assess shedding
- Review of family history
- Blood tests when needed
Doctors may order tests for ferritin, thyroid levels, and hormones. These tests help exclude reversible causes.
Ludwig Scale Explained
The Ludwig scale classifies female pattern hair loss into stages. It helps track progression and treatment response.
| Stage | Description |
|---|---|
| Stage I | Mild widening of part |
| Stage II | Noticeable thinning on crown |
| Stage III | Advanced thinning with scalp visibility |
Women in early stages respond better to medical treatment.
When Medical Treatment Makes Sense First
Most women do not need surgery at the start. Medical therapy remains the first-line approach for FPHL. Doctors recommend it before considering hair transplantation.
Medical treatment works best when:
- Hair follicles remain active
- Hair loss shows slow progression
- Donor hair is not yet stable
- The scalp still has miniaturized hair
Medications can thicken existing hair. They slow further loss. They do not create new follicles.
Why Early Surgical Decisions Can Fail
Hair transplantation does not stop ongoing hair loss. Surgery only relocates follicles. If hair loss continues, transplanted hair may look isolated. Density may appear uneven.
Doctors avoid surgery when:
- Hair loss remains unstable
- Diffuse thinning affects donor area
- Medical treatment was never tried
- Expectations remain unrealistic
Clinical guidelines emphasize stabilization before surgical planning.
Psychological Impact of Female Hair Loss
Hair loss affects confidence and emotional health. Many women experience anxiety and social withdrawal. Early counseling helps set realistic goals.
Doctors should explain:
- Treatment timelines
- Expected improvements
- Maintenance needs
- Long-term commitment
Clear communication improves satisfaction.
Medical treatment forms the backbone of female pattern hair loss management. Most women achieve visible improvement without surgery. Doctors always recommend medical therapy first because it stabilizes hair loss and improves hair quality.
What Medical Treatments Work for Female Pattern Hair Loss?
Medical therapy targets follicle miniaturization and growth cycle disruption. These treatments do not create new follicles. They strengthen existing ones and slow further loss.
First-Line Medical Treatment
Topical minoxidil remains the gold standard treatment for female pattern hair loss. Regulatory authorities approve it specifically for women.
Minoxidil:
- Prolongs the growth phase
- Increases hair shaft thickness
- Improves scalp blood flow
Doctors usually recommend:
- 2% solution twice daily, or
- 5% foam once daily
Consistency matters more than concentration. Missed applications reduce results.
Clinical guidance from Cleveland Clinic confirms that most women see early improvement within four months. Peak results appear around twelve months.
What to Expect After Starting Minoxidil
Patients often panic during the first eight weeks. Shedding may increase. This phase is temporary. It indicates follicles entering a new growth cycle.
| Timeline | Expected Change |
|---|---|
| 0–8 weeks | Temporary shedding |
| 3–4 months | Reduced hair fall |
| 6 months | Improved density |
| 12 months | Maximum response |
Stopping treatment reverses gains. Doctors stress long-term use.
Oral Medications for Female Hair Loss
Doctors prescribe oral treatments when topical therapy alone fails. These medications require supervision.
Oral Minoxidil
Low-dose oral minoxidil has gained popularity. Doctors prescribe it off-label in controlled doses.
Benefits include:
- Better compliance
- Uniform scalp coverage
- Reduced irritation
Possible side effects include ankle swelling and facial hair growth. Doctors adjust doses to minimize risk.
Anti-Androgen Therapy
Some women show increased sensitivity to androgens. Anti-androgens reduce this effect.
Common options include:
- Spironolactone
- Finasteride (selected cases only)
Doctors avoid these medications during pregnancy. Regular monitoring remains essential.
Guidelines from the International Society of Hair Restoration Surgery support combination therapy for appropriate patients.
Supportive and Adjunct Treatments
Adjunct therapies enhance medical results. They do not replace primary treatment.
Platelet-Rich Plasma (PRP)
PRP therapy uses growth factors from the patient’s blood. Doctors inject it into thinning areas.
PRP may:
- Improve hair thickness
- Reduce shedding
- Enhance transplant outcomes
Most protocols involve three sessions spaced one month apart.
Low-Level Laser Therapy (LLLT)
Laser devices stimulate follicular activity. Patients use them at home.
Benefits include:
- Improved hair density
- Minimal side effects
- Easy maintenance
Results remain modest but supportive.
Medicated Shampoos and Scalp Care
Ketoconazole shampoo reduces scalp inflammation. Healthy scalp improves follicle function.
Doctors recommend:
- Ketoconazole shampoo twice weekly
- Gentle cleansing routines
- Avoiding harsh styling practices
How Doctors Measure Treatment Response
Doctors track progress objectively. Visual improvement alone is not enough.
Response Evaluation Methods:
- Standardized photographs
- Hair density measurements
- Patient shedding logs
- Scalp examination
Doctors usually reassess after six months. They adjust therapy based on response.
| Response Level | Next Step |
|---|---|
| Good response | Continue medical therapy |
| Partial response | Add adjunct treatments |
| Poor response | Re-evaluate diagnosis |
| Stable but thin | Discuss surgical options |
When Medical Treatment Alone Is Enough
Medical therapy works best in early to moderate hair loss. Many women maintain satisfactory density for years.
Medical treatment alone suits women who:
- Have mild to moderate thinning
- Show active follicles
- Accept gradual improvement
- Commit to long-term care
These patients rarely need surgery.
When Medical Therapy Reaches Its Limit
Some women experience stabilization without cosmetic improvement. Hair loss stops but density remains low.
Doctors consider additional options when:
- Hair loss remains stable for 12 months
- Medical therapy shows limited thickening
- Donor hair appears healthy
- Patient expectations remain realistic
This point marks the transition toward surgical discussion. Medical therapy still continues even if surgery becomes an option.
Importance of Patience and Compliance
Hair treatment requires time. Short-term decisions lead to poor outcomes. Doctors stress discipline and follow-up.
Patients must understand:
- Hair grows slowly
- Results take months
- Maintenance never stops
Education improves compliance. Compliance improves results.
Hair transplant becomes a consideration only after doctors stabilize female pattern hair loss. Surgery does not treat the disease. It only redistributes healthy follicles. Correct timing protects natural results.
When Hair Transplant Becomes a Valid Option
Hair transplant works best for selected women. Doctors never recommend it as the first step. They consider surgery only after medical therapy reaches its maximum benefit.
A woman may qualify for a transplant when:
- Hair loss remains stable for at least twelve months
- Medical treatment no longer improves density
- Donor hair appears strong and permanent
- Thinning follows a recognizable pattern
- Expectations remain realistic
Doctors confirm stability through photographs and scalp exams. They avoid surgery during active shedding phases.
Why Diffuse Thinning Needs Extra Caution
Diffuse thinning affects large scalp areas. Many women lose density even in donor zones. This pattern increases surgical risk.
Transplant may fail when:
- Donor hair shows miniaturization
- Density looks poor at the back of the scalp
- Hair loss progresses rapidly
- Medical therapy was never optimized
In such cases, surgery may worsen appearance. Doctors prefer continued medical care or camouflage strategies.
How Surgeons Evaluate Female Transplant Candidacy
Surgeons perform a detailed assessment before approval. This process differs from male pattern baldness evaluation.
Evaluation includes:
- Donor density measurement
- Hair shaft thickness analysis
- Scalp laxity assessment
- Pattern mapping of thinning zones
- Review of treatment history
Clinical guidance supported by dermatology associations such as the American Academy of Dermatology emphasizes cautious selection in women.
Hair Transplant Techniques Used for Women
Doctors choose techniques based on hair loss pattern, styling habits, and donor quality.
Follicular Unit Extraction (FUE)
FUE involves removing individual follicles. Surgeons implant them into thinning areas.
Advantages:
- No linear scar
- Faster recovery
- Suitable for shorter hairstyles
Limitations:
- Limited graft yield per session
- Higher risk if donor is weak
Follicular Unit Transplantation (FUT)
FUT involves removing a thin scalp strip. Surgeons dissect follicles under magnification.
Advantages:
- Higher graft numbers
- Better for extensive thinning
- Preserves donor density
Limitations:
- Linear scar
- Longer healing time
Doctors choose technique based on safety, not trend.
Common Areas Treated in Female Hair Transplant
Female transplants focus on density improvement rather than full coverage.
Typical targets include:
- Central part line
- Crown thinning
- Frontal density behind hairline
- Temporal recession support
Surgeons rarely lower the frontal hairline aggressively. Natural balance remains the priority.
Expected Results and Timeline After Surgery
Hair transplant results take time. Patients must remain patient.
| Time After Surgery | What Happens |
|---|---|
| 1–2 weeks | Shedding of transplanted hair |
| 3 months | Early regrowth begins |
| 6 months | Noticeable density improvement |
| 12 months | Final cosmetic result |
Transplanted hair grows permanently. Native hair still needs medical support.
Risks and Limitations Women Must Understand
Hair transplant is safe when performed correctly. Still, it has limits.
Possible risks include:
- Shock loss of surrounding hair
- Uneven density
- Visible scalp if loss progresses
- Need for additional sessions
Doctors reduce risks through conservative planning and continued medication.
Why Medical Treatment Must Continue After Transplant
Hair transplant does not stop female pattern hair loss. Native hair may continue thinning.
Doctors insist on:
- Ongoing minoxidil use
- Anti-androgen therapy when indicated
- Periodic PRP or supportive care
Combination therapy protects both transplanted and native hair.
When Hair Transplant Should Be Avoided
Doctors refuse surgery when risks outweigh benefits.
Transplant should not proceed when:
- Hair loss remains active
- Donor hair appears unstable
- Expectations focus on instant results
- Patient avoids medical therapy
Ethical practice protects long-term outcomes.
Psychological Readiness Matters
Hair restoration affects self-image. Surgeons evaluate emotional readiness.
Patients must understand:
- Surgery enhances density, not perfection
- Results appear gradually
- Maintenance continues for life
Proper counseling improves satisfaction.
Choosing between medical treatment and hair transplant requires logic, patience, and expert guidance. A clear framework helps women avoid rushed decisions and protects long-term results.
How to Decide: Medical Treatment, Transplant, or Both
Doctors follow a structured decision path. This approach improves outcomes and reduces regret.
Step-by-Step Decision Framework
| Question | If YES | If NO |
|---|---|---|
| Is the diagnosis confirmed as FPHL? | Proceed to treatment planning | Treat reversible cause first |
| Has medical therapy run for 6–12 months? | Assess response | Start or optimize medical care |
| Is hair loss stable for at least 12 months? | Consider surgery | Continue medical therapy |
| Is donor hair strong and permanent? | Evaluate transplant candidacy | Avoid surgery |
| Are expectations realistic? | Plan conservatively | Counsel or defer |
This framework keeps decisions objective. It also aligns with best clinical practice.
What Combination Treatment Looks Like in Real Life
Most women benefit from a combined approach. Medical therapy preserves native hair. Surgery adds density where needed.
A typical plan includes:
- Continuous minoxidil use
- Anti-androgen therapy when indicated
- PRP as a supportive option
- Conservative transplant for density
- Long-term follow-up and adjustments
Combination care delivers stable and natural results.
Cost Considerations and Practical Planning
Costs vary by country, clinic, and graft count. Women should plan financially before surgery.
Factors That Influence Cost
- Number of grafts required
- Technique used (FUE vs FUT)
- Surgeon experience
- Clinic infrastructure
- City and country
Medical therapy also has ongoing costs. Patients should factor this into long-term planning.
General Cost Planning
| Component | Frequency |
|---|---|
| Medical therapy | Monthly / ongoing |
| PRP sessions | 3–4 per year (optional) |
| Hair transplant | One or staged sessions |
| Follow-up visits | 2–4 per year |
Clinics should provide itemized estimates. Transparency builds trust.
Recovery and Lifestyle After Treatment
Recovery timelines differ for medical therapy and surgery.
After Medical Therapy
- No downtime
- Daily compliance required
- Results appear gradually
After Hair Transplant
- Mild swelling for a few days
- Scab shedding within two weeks
- Normal activities resume in 7–10 days
- Visible regrowth starts by three months
Patients should avoid tight hairstyles and harsh chemicals during recovery.
Long-Term Maintenance Is Not Optional
Female pattern hair loss is chronic. Maintenance protects results.
Long-term care includes:
- Continued medical therapy
- Periodic scalp evaluation
- Lifestyle support for hair health
- Early intervention if shedding increases
Stopping treatment reverses gains. Doctors emphasize consistency.
Common Mistakes Women Should Avoid
Mistakes reduce outcomes and increase costs.
Avoid:
- Choosing surgery without stabilization
- Expecting instant density
- Ignoring donor limitations
- Stopping medication after surgery
- Comparing results with male transplants
Education prevents disappointment.
Final Clinical Perspective
Medical treatment remains the foundation of female hair loss management. Hair transplant works as a supportive tool. Proper timing, patient selection, and ongoing care determine success.
Women who follow a structured approach achieve natural, stable, and lasting improvement.
Frequently Asked Questions
Female pattern hair loss is a genetic condition that causes gradual thinning over the crown and mid-scalp while preserving the frontal hairline.
Yes. Medical therapy should always come first to stabilize hair loss and assess response.
Doctors usually recommend at least 6–12 months of consistent treatment before considering surgery.
Only selected cases qualify. Donor hair must be strong and stable.
No. Surgery does not stop the disease. Medical treatment must continue.
Yes. Long-term use is safe and necessary to maintain results.
Doctors use them when hormonal sensitivity contributes to hair loss and no contraindications exist.
Results look natural when surgeons plan conservatively and combine surgery with medical care.
No. Stopping medication can lead to loss of native hair around transplanted areas.
A woman with stable hair loss, adequate donor hair, realistic expectations, and commitment to maintenance.








